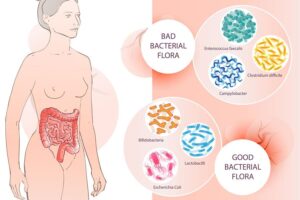
It is common knowledge that over 90% of the neurotransmitter serotonin is produced in the gut from cells that interact with the gut bacteria present in the colon. Depression after a course or two of antibiotics occurs in up to 22% of patients probably due to the alteration of healthy gut bacteria from the antibiotic.
Lowered levels of serotonin are commonly found in people with depression. In fact, one of the most widely known drugs to “treat” depression is Prozac, which has as its mechanism of action the poisoning of the pump in the nerve cell ending, which results in increased levels of serotonin in the nerve cell junction. The annual sales of this drug are in excess of $2 billion per year. So this is not a small problem in healthcare.
In our clinic, LifeWorks Wellness Center, we routinely test for levels of serotonin when treating patients who complain of depression. In the many years of doing these tests, I have never seen the serotonin level on urine testing be restored to normal by people taking Prozac or other drugs in the same class, called SSRIs (Selective Serotonin Reuptake Inhibitors). When we use a nutritional support program to improve serotonin levels using a healthy organic Paleo type diet, supplementation of amino acids and vitamins, and rebuilding of healthy gut bacteria with probiotics like Perfect Immune Defense, we usually get depression to be a thing of the past.
For a long time it confounded me why people who were taking SSRI’s didn’t have their serotonin levels restored to normal? Virtually all people that we have tested who had been taking the drug for many years still had well below normal levels. Could it be that Prozac and other SSRIs could be causing toxicity to the gut bacteria and that was the reason they didn’t correct the serotonin levels on our testing?
Then recently I ran across a new study in mice led by UCLA biologists that strongly suggests that drugs that target serotonin, such as anti-depressants, can have a detrimental effect on the gut’s microbiota.
This research confirms results from a growing number of studies reporting that anti-depressants can alter the gut microbiota that results in a detrimental effect on serotonin production. If the drug poisons certain gut bacteria, and they are key to the production of healthy serotonin levels, then that could be the reason why the drug never restored a healthy serotonin level in the patient.
Since this is a consistent finding, it started to make sense and this looks like what is happening. The drug will not restore or heal a lowered serotonin level, quite the opposite. It will damage the microbiome such that the body can not again produce a healthy serotonin level because of the gut biome damage.
My goal in treating a depressed patient is to restore their normal levels of neurotransmitters. Then they won’t be depressed if that is the cause of their problem. The drug is a crutch for those that it works in, but in my mind a very dangerous one.
All drugs, including antidepressants, are poisons of one kind or another and one must be very careful in using them long term. This is especially true when these drugs are often added to combinations of other drugs for diabetes, high blood pressure, cholesterol, GERD and others. The effects of the combinations of these drugs on gut bacteria is unstudied and unknown. But we do know that the more drugs the patient is on, the more he is likely to get serious side effects, including damage to his gut bacteria.
Nearly all modern research is pointing to the fact that health is, to a very large extent, dependent on a healthy microbiome. Drugs that affect our cells in the symptomatic treatment of some disease condition will certainly also affect our gut bacteria. They are living organisms and will be affected by drugs the same as our cells. How and to what extent? No one knows and almost no one seems to care! But if you are depressed and you are being prescribed another drug for that, you should care. It could hurt you.
A proven way to improve depression includes restoration of healthy gut bacteria through supplementation and correction of amino acid deficiencies, and probiotic usage. Also, in clinical studies, exercise consistently works as well as or better than drug therapy for depression. Maybe too, some help in the area of dealing with life stressors would surely make a difference.
About one in ten Americans aged 12 and over takes antidepressant medication.¹
Is there a better way to treat depression? We know the key is in the restoration of a healthy gut. Seems that modern research is confirming what has been known for almost a century. In the words of the great inventor Thomas Edison in 1903: “The doctor of the future will give no medicine, but will interest his patient in the care of the human frame, in diet and in the cause and prevention of disease.”
Great advice then and great advice now.
Have a great week.
Dr. David I Minkoff, MD
¹ CDC – National Center for Health Statistics No. 76, October 2011
Patient Testimonial
“I came to LifeWorks a year ago to get a Myers’ Cocktail and after learning from Tamora what they do at the clinic, I decided that this is the place the universe wanted me to be. I had been suffering from a long list of health issues, the most difficult being anxiety, panic attacks and depression. During my first consultation with the doctor, he took all the time I needed to tell my story and he told me how to heal. It had been a long road getting here, with years of seeing countless doctors with no answers other than “take this pharmaceutical and good luck”. At LifeWorks, I finally found a place of healing and somewhere that could put all the pieces of my puzzling story together. This is a place that is saving my life. My heartfelt thanks to everyone at the center for your loving and caring ways.” – H. M.